bcbs michigan inpatient prior authorization form
|
Provider Overview
• Pre-service or prior authorization is obtained – unauthorized transitions should be rare and justified • Acute Care provider secures the authorization |
|
Provider preauthorization and precertification requirements
23 jan 2024 · Providers can submit prior authorization requests for Blue Cross Blue Shield of Michigan Contracted Michigan provider acute inpatient |
|
State Health Plan Medicare Advantage Benefits
• In November Blue Cross will mail a pre-enrollment packet to members Prior authorization for certain services is key to making sure you receive |
|
MESSAs list of services requiring mandatory prior authorization
Inpatient residential or partial hospital (non-participating facility) Yes Blue Cross Behavioral Health Refer to Blue Cross Blue Shield of Michigan |
|
BLUE CROSS BLUE SHIELD OF MICHIGAN PLAN
PRIOR AUTHORIZATION REQUIRED Prior authorization is a drug class management technique that requires select prescriptions to meet defined criteria before |
|
Blue Cross Complete of Michigan authorization requirements
Inpatient admissions Services require authorization This includes long-term acute care inpatient rehabilitation and skilled nursing care Blue Cross Complete |
|
Acute inpatient hospital assessment form
Complete this form and submit it along with supporting clinical documentation when requesting authorization for admissions to and extensions of stays at acute |
|
Your Benefit Guide
The inpatient admission and length of stay must be medically necessary and pre-approved The claim form is available from your BCBSM Service Center the |
When submitting either of these forms to BCBSTX, please use the following applicable fax # or address: Fax 888-579-7935.
If unable to fax, mail to: BCBSTX, P.O.
Box 660044, Dallas, TX 75266-0044.
|
MPB Group PPO Non-Michigan Acute Inpatient Fax Assessment Form
Precertification isn't a guarantee of payment. Facilities and other health care providers must verify patient eligibility and benefits prior to making. |
|
Acute Hospital Request Form
Precertification does not guarantee payment. HUMAN ORGAN TRANSPLANT. Contact name. Title. Acute Inpatient. Fax Assessment Form. InterQual criteria MET. |
|
BCBSM Request for Preauthorization Form
Blue Cross Blue Shield of Michigan Request for Preauthorization Form. Most preauthorization requests can be resolved by contacting Provider Relations and |
|
Provider Preauthorization and Precertification Requirements for
28-Jan-2022 Blue Cross Blue Shield of Michigan Commercial Products (Non-Medicare). Precertification is required for: • Psychiatric inpatient admissions. |
|
MPB Group PPO Non-Michigan Acute Inpatient Fax Assessment Form
Precertification isn't a guarantee of payment. Facilities and other health care providers must verify patient eligibility and benefits prior to making |
|
Provider Preauthorization and Precertification Requirements for
04-Aug-2022 Requests for inpatient authorization for Blue Cross Blue Shield of Michigan ... appropriate assessment form and submit the request via fax. |
|
Skilled Nursing Facility Acute Inpatient Rehabilitation Facility Fax
Please verify eligibility and benefits prior to request. Fax Assessment Form ... Please allow 24-48 hours for processing precertification and ... |
|
Provider Preauthorization & Precertification Requirements
Behavioral Health. Commercial Blue Cross Blue Shield of Michigan Products-Non-Medicare. Precertification is required for: • Psychiatric inpatient admissions. |
|
Medicare Plus Blue PPO Provider Manual
01-Jan-2022 Blue Cross Blue Shield of Michigan is a nonprofit corporation and ... Prior authorization of outpatient radiation oncology services and ... |
|
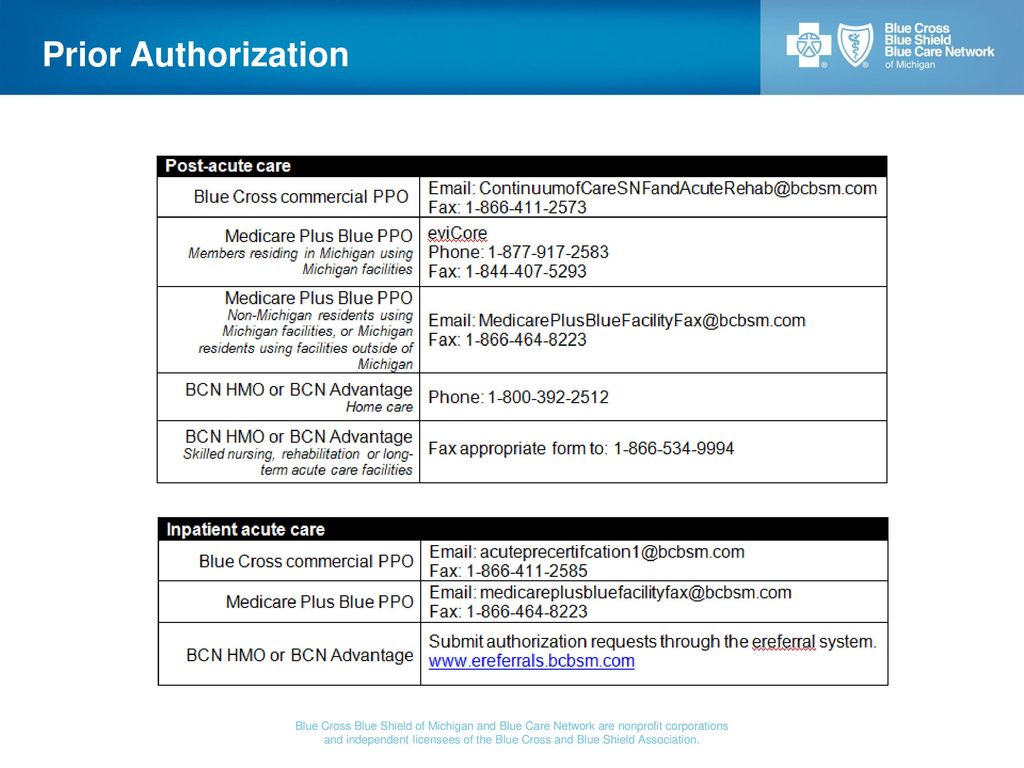
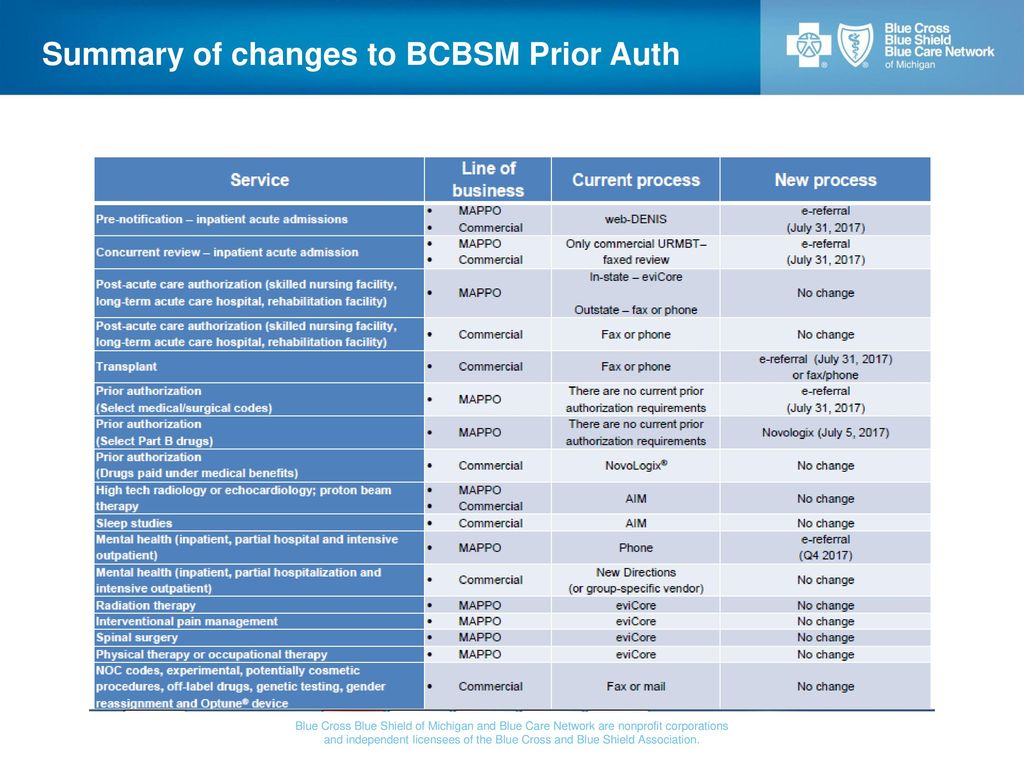
Blue Cross and BCN: Submitting prior authorization requests for
For BCN commercial and BCN Advantage admissions complete the Request for · Review of Initial Inpatient Admission form and attach it to the case in the e- |
|
Acute Inpatient Fax Assessment Form - Blue Cross Blue Shield of
Please allow 24-48 hours for processing precertification and recertification requests Precertification All Commercial LTAC requests must be submitted on LTAC form BCBSM offers case management assistance for discharge planning |
|
Provider Preauthorization & Precertification Requirements
whether he or she meets BCBSM criteria for treatment in the inpatient setting Precertification request forms and instructions for submission are located at: |
|
Bcbs of michigan prior authorization form - Squarespace
Blue Cross Blue Shield of Michigan uses the following pre-certification and Qualified Nursing, Inpatient Rehabilitation and Long-Term Acute Care for Michigan |
|
Bcbs of michigan ppo prior authorization form - Squarespace
For more information, see our FAQ( PDF) Skilled nursing, inpatient rehabilitation and long-term acute care for non-Michigan service providers and members pre- |
|
Blue Cross Complete of Michigan authorization requirements
This includes long-term acute care, inpatient authorization requests using the Blue Cross Complete Medication Prior Authorization Request form, which is |
|
Blue Cross Complete authorization requirements
30 sept 2020 · This includes long-term acute care, inpatient rehabilitation and skilled Authorization request must be submitted at least 14 days prior to service Cross Complete Medication Prior Authorization Request form, which is |
|
Post-Acute Care Utilization Program for Blue Cross Blue - eviCore
eviCore is an independent company that manages prior authorization for Blue Cross and Blue Shield of Michigan Page 2 Agenda ➢Post-Acute Care Program |
|
Post-Acute Care Frequently Asked Questions Program - eviCore
EviCore healthcare will manage only Blue Cross Blue Shield of Michigan Medicare Plus BlueSM PPO Inpatient rehabilitation facilities and long- Instructions to appeal the precertification decision are located in the denial letter This will be |
|
Your Benefit Guide - State of Michigan
Blue Shield of Michigan (BCBSM) under the direction of the Michigan Civil other forms of toxic metal poisoning You may obtain pre-surgical consultations if the surgery will take place in an inpatient or outpatient hospital A description of any prior authorization requirements and any limitations, restrictions or exclusions |
|
Authorization Requirements - Blue Cross Blue Shield
To obtain an authorization, Blue Cross Blue Shield of Prior authorization is required when the service is provided for inpatient Management consent form and tentative treatment and discharge plan before admission; 2) the services meet |