bcbs standard prior authorization form
|
Instructions for Completing
This form should be used when authorizing Blue Cross Blue Shield of Illinois (BCBSIL) to disclose an individual's protected health information (PHI) to a |
|
Standard Authorization Form
II Authorization and Purpose: I request and authorize Blue Cross and Blue Shield of Oklahoma to disclose my protected health information as described |
|
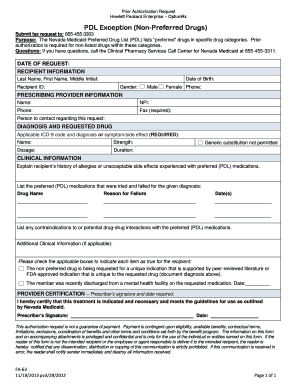
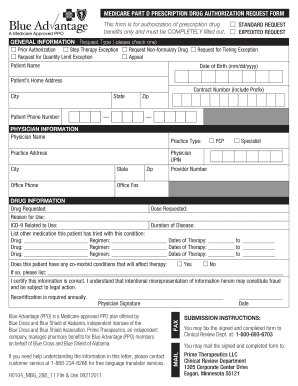
Standard Drug Prior Authorization Form
I certify that the information provided is accurate and complete to the best of my knowledge and I understand that any falsification omission or concealment |
|
Pre-certification / Pre-Authorization Request Form
Pre-certification / Pre-Authorization Request Form For Procedures and Date form completed: Phone: Fax: Admitting physician name: Admitting physician NPI |
|
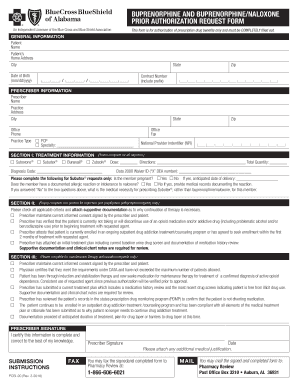
Prior authorization
Certain medical services and treatments need prior authorization before you receive care Basic Option and Standard Option You must obtain prior approval for |
|
434 Massachusetts standard form for Medication Prior Authorization
This form is being used for: Check one: □ Initial Request ☐ Continuation/Renewal Request Reason for request (check all that apply) |
How do I start pre authorization?
The patient or their representative can contact their insurance company and provide the relevant information to start the Prior Authorization process.
It's best to confirm with the healthcare provider if they have the information and are willing to submit the request.Providers also have the option to use electronic prior authorization, or complete the California standard Prescription Drug Prior Authorization Request Form and fax to (888) 697-8122.
What is authorization request form?
An authorization form is a document that is duly endorsed by an individual or organisation which grants permission to another individual or organisation to proceed with certain actions.
It is often used to grant permission to carry out a specific action for a fixed period of time.
What is the number for prior authorization for BCBS Illinois?
Prior Authorization/Utilization Management Blue Cross and Blue Shield of Illinois.
This page may have documents that can't be read by screen reader software.
For help with these documents, please call 1-877-774-8592.
|
434 Massachusetts standard form for Medication Prior Authorization
Prior Authorization Step Therapy |
|
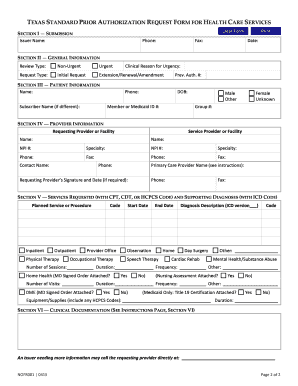
Texas Standard Prior Authorization Request Form for Health Care
Texas Standard Prior Authorization. Request Form for Health Care Services. NOFR001 |
|
MASSACHUSETTS STANDARD FORM FOR MEDICATION PRIOR
Reason for request (check all that apply): D Prior Authorization Step Therapy |
|
Michigan Prior Authorization Request Form for Prescription Drugs
when a policy certificate or contract requires prior authorization for prescription drug benefits. A standard form |
|
Texas Standard Prior Authorization Request Form for Prescription
Beginning September 1 2015 |
|
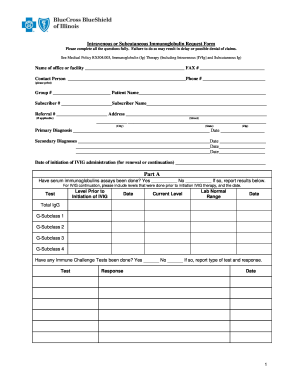
MASSACHUSETTS STANDARD FORM FOR SYNAGIS® PRIOR
Massachusetts Standard Form for Synagis® Prior Authorization Requests ... *Some plans might not accept this form for Medicare or Medicaid requests. |
|
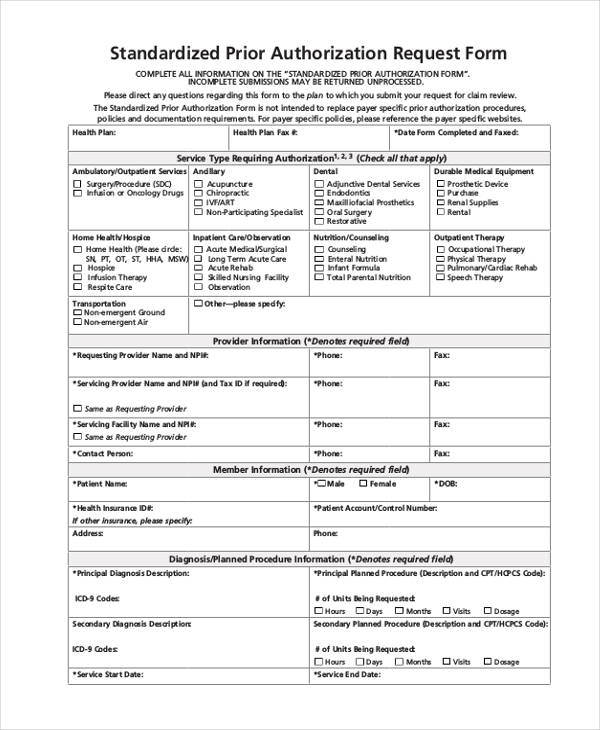
Introducing: Standardized Prior Authorization Request Form
1 Mei 2012 The Standardized Prior Authorization Form is not intended to replace payer ... Massachusetts Medical Society Blue Cross Blue Shield. |
|
NEW HAMPSHIRE UNIFORM PRIOR AUTHORIZATION FORM
health accreditation standards for urgent care in that adherence to the standard timelines: a) could seriously jeopardize the life or health of the patient or |
|
Using Standard Prior Authorization Forms when Reviewing
9 Agu 2016 Commercial Health Insurers; Blue Cross Blue Shield of ... Massachusetts Standard Form for Medication Prior Authorization Request. |
|
Tufts
1 Nov 2015 The Standardized Prior Authorization Form is not intended to replace payer ... Massachusetts Medical Society Blue Cross Blue Shield. |
|
434 Massachusetts standard form for Medication Prior Authorization
Prior Authorization, Step Therapy, Formulary Exception □ Quantity Health Plan or Prescription Plan Name: Blue Cross Blue Shield of Massachusetts |
|
Pharmacy Prior Authorization Request Form - Blue Cross Blue
Fax completed prior authorization request form to 602-864-3126 or email to Blue Cross Blue Shield of Arizona, Mail Stop A115, P O Box 13466, Phoenix, AZ 85002- approved by BCBSAZ expired) Turn-Around Time For Review Standard |
|
Drug Prior Authorization Request Form
Drug Prior Authorization Request Form (1)* Insurer: (2)* Date: Member Information (3) Group#: (4) Member#: (5) Name of Insured: (6)* Patient Name, Last: |
|
Standard Authorization Form to Release Protected Health
Instructions for Completing Standard Authorization Form to Use this form to authorize Blue Cross and Blue Shield of Illinois (BCBSIL) to disclose your protected health information (PHI) to a Includes any information related to pre- service, |
|
NEW HAMPSHIRE UNIFORM PRIOR AUTHORIZATION FORM
Insurer or Pharmacy Benefit Manager (PBM) Name: Anthem Blue Cross and Blue Shield Electronic Prior Authorization Webpage: https://providerportal surescripts net/ adherence to the standard timelines: a) could seriously jeopardize the |
|
Michigan Prior Authorization Request Form for Prescription Drugs
A standard form, FIS 2288, is being made available by the Department of Prior authorization requests are defined as requests for pre-approval from an insurer for □Priority □Magellan □Blue Cross Blue Shield of Michigan □HAP □ |
|
Prior Authorization/Precertification Request - MN BCBS Provider
Blue Cross and Blue Shield of Minnesota and Blue Plus (Blue Cross) prior To prevent delay in processing your request, please fill out this form in its entirety with all standard timeframe was applied it may seriously jeopardize the member's |
|
Prior Authorization Fax Form - MyPrimecom
Start saving time today by filling out this prior authorization form electronically xpedited/Urgent review – prescriber certifies that waiting for a standard review could an Independent Licensee of the Blue Cross and Blue Shield Association |