abn modifiers medicare
|
MLN006266 Medicare Advance Written Notices of Non-coverage
Advance Beneficiary Notice of Non-coverage (ABN) (CMS-R-131) — All health care providers and suppliers must issue an ABN when they expect a payment denial that transfers financial liability to the patient This includes: |
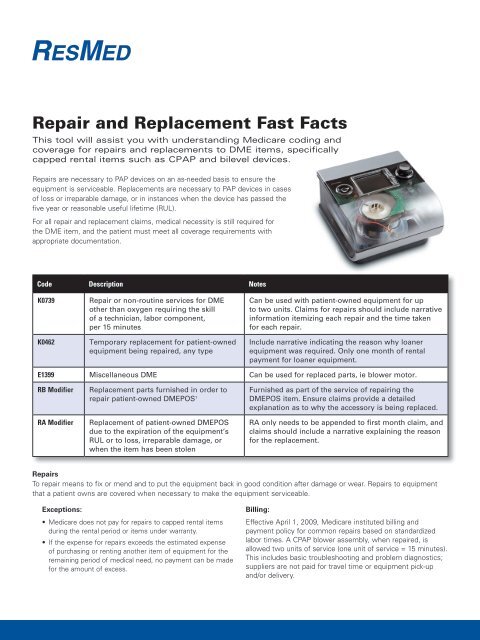
What are Medicare advance beneficiary notice – ABN modifiers?
Modifiers GA GX GY and GZ are HCPCS Level II most commonly used Medicare Advance Beneficiary Notice – ABN modifiers. Let us know about the description of above ABN modifiers and instructions to use with a CPT code, but before moving to that part first let us learn the term ABN –Advance Beneficiary Notice.
How do I report Medicare if I don't have an ABN?
Report Medicare statutorily excludes the item or service, or the item or service doesn’t meet the definition of a Medicare benefit. Use this modifier combined with modifier –GX. Report when you expect we’ll deny payment of the item or service because it’s medically unnecessary and you didn’t issue an ABN.
What Medicare modifiers do you use?
These are the top 4 Medicare modifiers we use. Waiver of Liability Statement Issued as Required by Payer Policy. This modifier indicates that an ABN is on file and allows the provider to bill the patient if not covered by Medicare. automatically assign the beneficiary liability. Notice of Liability Issued, Voluntary Under Payer Policy.
What is a Medicare ABN & how does it work?
If applicable, the ABN must also specify the duration of the period of treatment. If during the course of treatment additional non-covered items or services are needed, the notifier must give the beneficiary another ABN. An ABN is a written notice a supplier gives to a Medicare beneficiary before providing an item and/or service.
|
MLN006266 – Medicare Advance Written Notices of Non-coverage
ABN Claim Reporting Modifiers . An advance written notice of non-coverage helps Medicare Fee-for-Service (FFS) patients choose. |
|
MLN006266 – Medicare Advance Written Notices of Non-coverage
ABN Claim Reporting Modifiers . An advance written notice of non-coverage helps Medicare Fee-for-Service (FFS) patients choose. |
|
MLN006266 – Medicare Advance Written Notices of Non-coverage
ABN Claim Reporting Modifiers . An advance written notice of non-coverage helps Medicare Fee-for-Service (FFS) patients choose. |
|
CMS Manual System - Pub 100-04 Medicare Claims Processing
04-Feb-2011 The GZ modifier indicates that an ABN was not issued to the beneficiary and signifies that the provider expects denial due to a lack of ... |
|
Medicare Payments for Part B Claims with G Modifiers (OEI-02-10
No ABN is required with the GY modifier. The provider or supplier may use this modifier when a beneficiary needs Medicare to deny the claim so that it can be. |
|
CMS Announces New ABN Modifiers How to use ABN Modifiers?
In 2009 the Centers for Medicare & Medicaid Services (CMS) implemented the use of Procedure Coding System (HCPCS) Level II modifiers related to ABN. |
|
Outpatient Therapy Services and Advance Beneficiary Notice of
modifier as a confirmation that services are medically necessary as justified by required to issue the ABN to original (fee-for–service) Medicare ... |
|
Medicare FFS Response to the PHE on COVID-19
08-Sept-2021 CMS requires the modifier or condition code. Submission of the modifier or ... Advance Beneficiary Notice of Non-Coverage (ABN)_CMS-R-131. |
|
Medicare Advance Written Notices of Noncoverage - CMS
ABN claim reporting modifiers ○ When not to use an advance written notice of noncoverage ○ Resources TYPES OF ADVANCE WRITTEN NOTICES OF |
|
CMS Announces New ABN Modifiers How to use ABN Modifiers?
In 2009, the Centers for Medicare Medicaid Services (CMS) implemented the use of the revised Advance Beneficiary Notice of Non-coverage (ABN) form, CMS- |
|
Medicare Payments for Part B Claims with G Modifiers - Office of
No ABN is required with the GY modifier The provider or supplier may use this modifier when a beneficiary needs Medicare to deny the claim so that it can be |
|
Advance Beneficiary Notice of Noncoverage (ABN)
information on claim modifiers associated with mandatory ABN use Common reasons for Medicare to deny an item or service as not medically reasonable and |
|
Modifiers GA, GX, GY, and GZ - Moda Health
5 mai 2014 · (CMS 1) In this memo CMS instructed: • An advanced beneficiary notice of non- coverage (ABN) is to be used for Medicare beneficiaries only • |
|
Advanced Beneficiary Notices - American Academy of Audiology
This modifier is to be used only when an ABN is required for covered services and should not be reported with any other Medicare modifier Mandatory ABNs are |
|
The following updates will affect Medicare Advantage:
with a GX and GY modifier (see below for modifier information) The ABN is given to beneficiaries enrolled in the Medicare Fee-For-Service (FFS) program It is |
|
Advance Beneficiary Notice of Noncoverage (ABN) - AAPC
of Noncoverage (ABN) (Form CMS-R-131) for all situations where Medicare payment is Level II modifiers to distinguish between voluntary and required ABNs |
|
ADVANCED BENEFICIARY NOTICE (ABN) - Office of Billing
The ABN allows the claim reviewed by Medicare and if payment is denied, the patient Use this modifier when you issue a mandatory ABN for a service or item |















![Mental Health Modifiers: The Definitive Guide [2020] Mental Health Modifiers: The Definitive Guide [2020]](https://0.academia-photos.com/attachment_thumbnails/43583444/mini_magick20190215-9385-1er6gsj.png?1550290656)






![MDS HIPPS Modifiers Cheat Sheet by [deleted] - Download free from MDS HIPPS Modifiers Cheat Sheet by [deleted] - Download free from](https://image.slidesharecdn.com/commonlyusedmedicaremodifiers-150805141123-lva1-app6892/95/commonly-used-medicare-modifiers-ga-gx-gy-gz-1-638.jpg?cb\u003d1440185477)


![Psychiatry CPT Codes: The Definitive Guide [+Cheat Sheet PDF] Psychiatry CPT Codes: The Definitive Guide [+Cheat Sheet PDF]](https://0.academia-photos.com/attachment_thumbnails/56918874/mini_magick20190111-9453-d6n6x.png?1547223233)

















![Psychiatry CPT Codes: The Definitive Guide [+Cheat Sheet PDF] Psychiatry CPT Codes: The Definitive Guide [+Cheat Sheet PDF]](https://docplayer.net/docs-images/41/18913106/images/page_8.jpg)